Houser was baffled. How could this woman have trouble breathing when her nose was wide open? And why would a cold make her feel less blocked? He described the situation to his attending physician, who then went into the room without Houser. After the appointment, the attending physician hemmed and hawed and never provided a good explanation. He told Houser not to worry about it.
But Houser did worry. What could explain such a bizarre condition? He did some research, and after talking to Dr. Murray Grossan, an ENT doctor in Los Angeles, he learned about empty nose syndrome, a controversial condition coined by the Mayo Clinic’s Dr. Eugene Kern in 1994. Kern described “nasal cripples” who, after turbinate surgery, suffered from symptoms like nasal dryness, crusting, and a sense of obstruction despite a wide-open nasal airway. With the help of colleagues, Kern conducted a study of 242 patients who’d been diagnosed with a rare type of nasal infection and theorized that many of these patients actually suffered from empty nose syndrome.
Not everyone in the ENT community was convinced by Kern. In a 2001 Los Angeles Timesarticle, one physician referred to the supposed illness as “empty head syndrome.” But Houser took to the internet and began talking with people about their ENS symptoms. In one forum, he started a “Questions for Dr. Houser” thread. Some in the forum sound merely curious (“Is it good for us to swim?”). Some wonder about stem cell treatment to replace missing tissue (“Your first goal, if you want stem cells or another treatment,” Houser responds, “should be to get ENS recognized as a problem.”). Others can’t sleep and are getting desperate (“I am devastated. … I can find things to do to make it through the day; can you help me make it through the night?”). Eventually there were so many questions — nearly 30 pages of threads — that Houser’s wife was getting mad at him for spending all night on the internet. He had to stop answering questions online, but he didn’t stop his investigation.
Once patients realized an ENT doc was not only interested in their condition but also wanted to help, they began traveling from Australia, Europe, China, and the Middle East to Houser’s clinic in Cleveland. For patients Houser diagnosed with ENS, he developed an AlloDerm implant to mimic the lost turbinate tissue. Insurance didn’t cover the $9,000 to $14,000 procedure, but it seemed to be working. One of Houser’s patients self-published a book about his ENS experience: Having Nasal Surgery? Don’t You Become an Empty Nose Victim! Houser wrote the foreword.
“I’ve had about a dozen patients tell me that I’ve saved their lives and kept them from committing suicide,” says Houser, who has operated on about 70 people. “That’s why I continue to do this, because, to be honest, these patients are very difficult.”
Since Kern’s report in 2001, very little had been written about empty nose until Houser published the findings of his experimental implants in 2007, and then another article — “The Diagnosis and Management of Empty Nose Syndrome” — in The Otolaryngologic Clinics of North America in 2009. In the same journal issue, Dr. Spencer Payne at the University of Virginia published a response paper titled “Empty Nose Syndrome: What Are We Really Talking About?”
“The problem with empty nose syndrome is probably not that it does not exist,” Payne writes, “it is that we cannot adequately explain its existence by what we currently understand about the nose. Many otolaryngologists are unwilling to make a ‘leap of faith’ and, instead of acknowledging the existence of something they do not understand, are left skeptical of it in its entirety.”
While the symptoms ENS patients complain of are unique, their plight is familiar. For years, people suffering from chronic fatigue syndrome were treated with skepticism from the medical community and often told their debilitating condition was psychogenic. “Maybe these people are just lazy” was the unspoken (or sometimes spoken) refrain. BuzzFeed previously reported on a 2010 CDC study that concluded chronic fatigue patients suffered disproportionately from “maladaptive personality features” like neuroticism, paranoia, and OCD. It wasn’t until 2015 that the National Academy of Sciences pronounced chronic fatigue syndrome to be a debilitating condition with concrete physical symptoms and not a psychological illness. In the same NAS study, most patients reported it taking more than a year to get a diagnosis; a third reported it took more than five years.
Fibromyalgia patients face similar skepticism. Physicians also once believed irritable bowel syndrome was a psychological condition. Leaky gut syndrome is accepted within some corners of alternative medicine, but many doctors are skeptical of its existence. Morgellons — a more recent controversial condition involving painful, itchy lesions with mysterious “fibers” — is often regarded as a delusion, a form of psychosis.
Regardless of the validity of these contentious conditions, the experience for people who believe they have them is similar. They go from doctor to doctor, craving a diagnosis, or at least a physician who will take their complaints seriously. In one study, chronic fatigue syndrome patients said that “lack of acknowledgment could be even worse than the symptoms.” Meanwhile, the actual symptoms — which are experientially real, even if the source is debated or unknown — persist. The longer the symptoms persist, the more likely they are to either exacerbate underlying psychological conditions (anxiety, depression, OCD) or create them.
To suffer is one thing. To suffer and be told by medical professionals that nothing is wrong? That’s enough to make some people want to end it all.
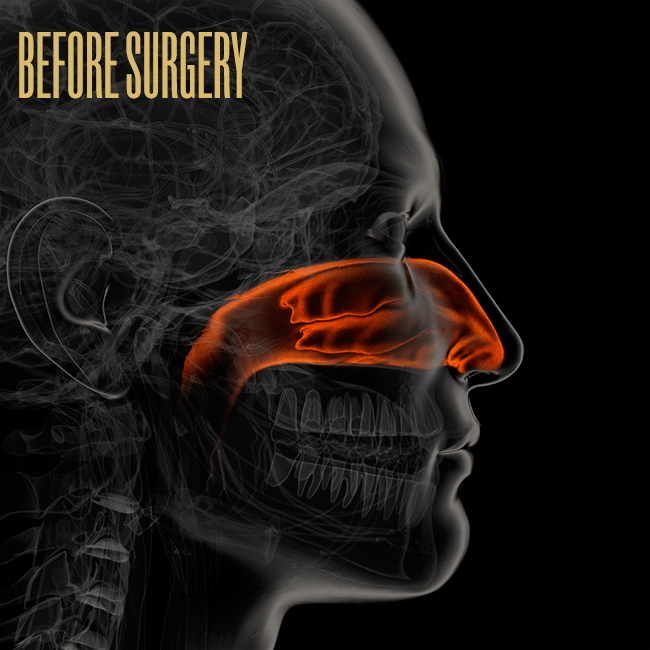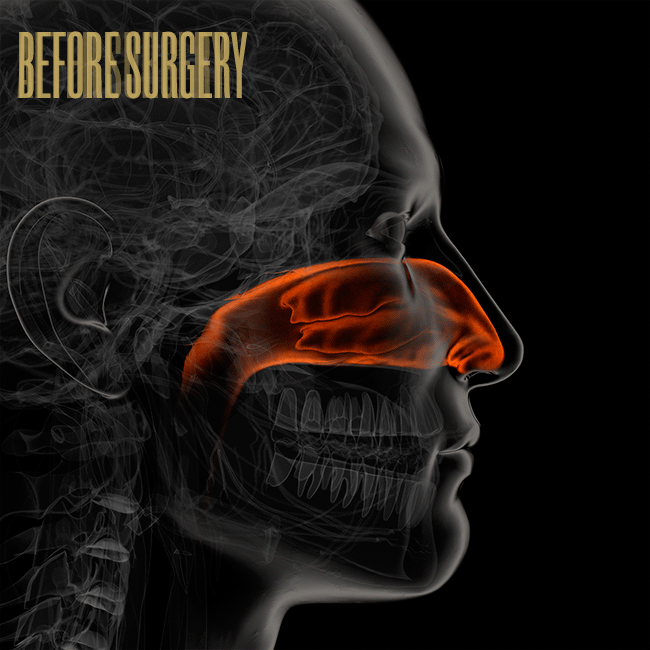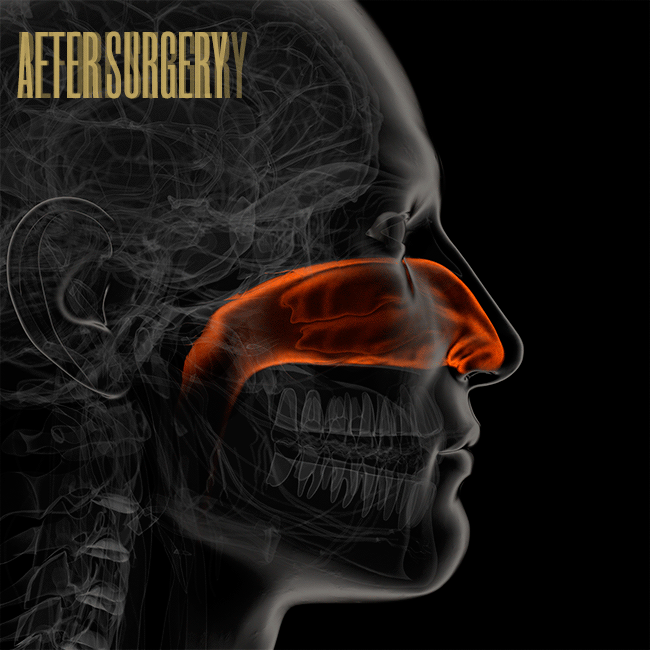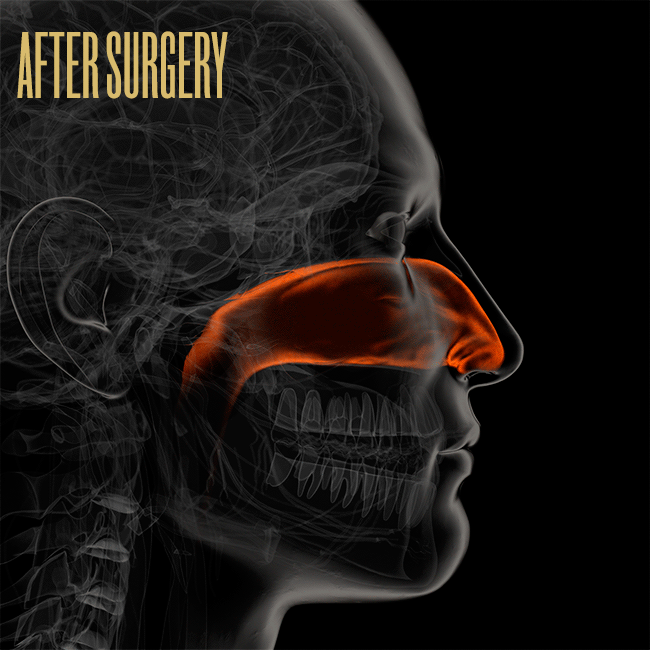
Inside your nose are two bony shelves divided by your septum, and these shelves contain three sets of turbinates. Each side of the nose contains a low, middle, and high turbinate. The low one, called an inferior turbinate, is the biggest — like a small cigar, about five or six centimeters long — and inside the inferior turbinate are blood vessels that can swell and shrink dramatically. (Imagine a penis and you’re not far off.) Turbinates help regulate airflow through the nose and also warm, filter, and humidify the air using a moist outer lining of tissue called mucosa.
Allergies, sinus infections, and other conditions can cause the inferior turbinate to stay enlarged, which leads to nasal blockage. If that’s the case, and if antibiotics don’t work, it’s not unusual for an otolaryngologist to recommend reducing the inferior turbinate (and, in rare cases, the middle turbinate). There are a number of ways to do that, and there’s no consensus on which method is best. Some doctors break the bone and move the structure out of the way. Some remove about one centimeter from the head of the turbinate. Some remove the bottom third of the entire tube. Others leave the outer tube alone and remove the inside, like taking the tobacco out of a cigar. Some doctors shrink the turbinate using cauterization or radio frequency. Sometimes doctors remove the entire turbinate — a total turbinectomy — though that method has fallen out of favor in the U.S. Often these procedures are done in combination with a septoplasty to fix a deviated septum.
Illustration by Bryan Christie
The CDC estimates that in 2006 (the most recent year of data), more than 900,000 people underwent nasal surgery. Though the CDC couldn’t provide data regarding turbinate surgeries specifically, the doctors I spoke to say a turbinate reduction is probably the most common procedure in rhinology, and they also say most of those patients walk away happy.
So imagine you’re an otolaryngologist operating on hundreds, maybe thousands, of patients. In follow-up appointments, almost all of them thank you for helping them to breathe normally for the first time in years. Only a handful are dissatisfied. One patient says he can’t breathe correctly. He feels like he’s suffocating. But everything looks great in his nose. The airway is completely open. The surgery did exactly what it was supposed to do.
And yet the patient keeps coming back, complaining more and more. He seems anxious, jittery, depressed. He’s not sleeping well. He’s having trouble performing everyday tasks. With each follow-up appointment, he becomes increasingly agitated. He says this routine surgery resulted in empty nose syndrome and ruined his life. You’ve heard of the condition, but you also know some doctors are skeptical of it. You certainly never spent time on the topic in medical school, where otolaryngology students concentrate on more common nasal problems, like sinusitis, deviated septum, and cancer. Not to mention the ears and throat.
Lots of other patients have appointments lined up, and they all take time. This outlier is taking time away from those patients. Eventually, you throw up your hands and discharge him from your practice.
There’s only one explanation: This patient is crazy.
Doctors like Houser in Cleveland, Payne at UVA, Jayakar Nayak at Stanford University, Subinoy Das at the U.S. Institute for Advanced Sinus Care and Research in Columbus, and researchers at Ohio State University are studying empty nose syndrome and trying to figure out why some patients get it and others don’t. Houser, Nayak, and Das treat ENS patients with implants and/or injections, and many of these patients have seen improvement. (Carol Helling says Brett received injections from Das but saw only temporary improvement; Das declined to comment for this story.)
Yet fundamental questions about ENS have yet to be answered. Are there environmental factors? Doctors in warm, humid climates like Singapore and Australia routinely perform total turbinectomies, and instances of ENS aren’t reported there as often, even though one study has shown that as many as 20% of patients who have their entire inferior turbinates removed could develop ENS.
And what accounts for the delayed diagnoses? Some patients begin experiencing symptoms months after the surgery; for others, symptoms don’t arise for years.
Dr. Jayakar Nayak Courtesy Jayakar Nayak
No one knows for sure why some turbinate reductions result in ENS and others don’t, but there are currently two prevailing theories. Houser’s theory argues that for ENS to occur, turbinate tissue must be removed or damaged, and then the sensory nerves in that area must regenerate poorly. Some methods of turbinate surgery can damage the nerve-rich mucosal layer more than others.
The other theory has to do with airflow — that the shape of a patient’s nose, and the way air flows through that nose, makes a patient more or less susceptible to ENS. Payne also thinks turbulence plays a role. “The more turbulent the airflow, the less you’re going to get a sense of good breathing,” he says. “It’s like if you stick your head out the window of a moving car, you can breathe in through your nose and feel the air moving through there, but I almost get anxious, because the air seems like it’s so poorly moving through the nose. I wouldn’t be surprised if in the empty nose patient, it’s not just a sense of decrease in receptors. It’s also an increase in the turbulence.”
The physics of airflow through the nose is complex and still not fully understood, though a study is underway at Ohio State University to better understand it. OSU’s Dr. Alex Farag and engineer/researcher Kai Zhao are developing 3D models to perform virtual nasal surgeries on patients before an actual surgery. By taking measurements and running models, they hope to see how the surgery could affect nasal airflow, which could lead to more-informed surgeries and fewer complications.
It could also be that both the airflow and mucosal/sensory theories are simultaneously true. For now, Houser and Stanford’s Nayak use cotton pledgets in the nose to help diagnose patients who complain of ENS symptoms. When the piece of cotton is inserted correctly, a patient with ENS will often feel radical improvement.
And then there’s the psychological mystery. Nayak says the ENS patients he has treated not only breathe better, they’re happier. “Anxiety, depression — all of these are off the charts for the initial patient with true empty nose syndrome,” Nayak says. He and his team are still trying to understand why that simple tubular structure seems to be essential to a proper sense of well-being for some people.
Houser can’t fully explain the relationship between mental health and ENS either. “I’ve wondered, which came first?” he says. “Were they that way, and therefore they’re more prone to nerves healing poorly after surgery and developing empty nose? Or is it the empty nose that made them so nervous and worried? I can say for sure that I’ve seen nervous, worried patients, and I implant them, and they do appear more at ease after they’re implanted. When I can get their breathing better, they’re less anxious.”
In a 2012 study in France, doctors treated a 37-year-old man with ENS symptoms who left his job and all social relationships. He spent most of his time alone in his bedroom with a humidifier. After doctors treated him with cognitive therapy and an antidepressant, many of his symptoms cleared up. “Treating ENS as a somatic symptom disorder might constitute a first-line safe alternative to surgical or even medical treatment,” the authors say.
“What we’ve seen in a lot of other chronic diseases is, each person’s perception of how bad they are is also dependent upon their general psychological health,” says UVA’s Payne. “People with poor coping mechanisms, with underlying depression or anxiety disorder — they are more likely to have symptoms that seem to take over their lives. That’s just not a normal response to chronic disease. And so you scratch your head, because as a physician, it’s the hardest thing trying to understand when are symptoms real, when are symptoms real but exacerbated by underlying psychological issues, and when are symptoms completely psychological.”
One ENS patient I spoke with, 52-year-old Sheila O’Shea, has become an informal counselor for suicidal ENS sufferers and sometimes fields late-night phone calls from them. She finds the emphasis on depression and mental health issues associated with ENS patronizing and insulting. “We’re sane people going through an insane situation,” she says. “Have you ever been stuck underwater, and you couldn’t make it to the surface fast enough? That panic you have? We have that all day long.”
She, like Brett, insists the accompanying mental condition is different from depression. “It’s as if you’re looking at the world through a big piece of Plexiglas. You can see everything and hear everything, but every experience is flat,” she says. “Depression messes with perception. Here, nothing is wrong with our perception. I’m not depressed.”
Brett Helling’s older brother, Paul, once gave him a mounted deer head he’d fished out of the trash. As a joke, Brett put the deer head in his car and drove around town with it for months. The first time Sean Gardner saw it, they were drinking beers on a Saturday afternoon in a friend’s living room. “Suddenly, this deer is banging its antlers against the window,” Sean says. “We’re all freaking out, like, ‘Oh my God!’ I run over to the side and I see Brett with this big smile. And he’s like, ‘Yeah, you just got deer-burned.’ That became his new thing.”
“He deer-burned me in the kitchen once,” Mollie Gardner says, laughing.
In the day or two following Brett’s death, Sean and Mollie wondered aloud, hopefully, if the whole ordeal was just another deer burn — the ultimate fake-out. But they knew that was wishful thinking. Once friends and family began arriving from out of town, Carol gave Sean and a few other friends one of several typed-in-advance notes Brett had left in his car near the bridge. There was also a handwritten note for the police.
“Suffering from empty nose syndrome (aka: sinus surgery gone wrong) and cannot suffocate any longer,” he’d scribbled with a Sharpie. “Please recognize this for what it really is and not just pass it off as ‘depression.’ … ENT doctors need to stop taking away perfectly good lives like mine was. This disease is very real, is untreatable, yet 100% preventable. Awareness is needed to make ENS a household name so people will stop being talked/pushed into very dangerous ‘routine’ surgery. We will continue to lose good, happy, productive, and healthy people to this disease otherwise. It took everything from me. I am not the last. http://www.emptynosesyndrome.org.
“P.S. Mom, I’m sorry! I held on as long as I could for you.”
The other notes went into more detail. One was a nearly 30-page script that Brett instructed Sean and three other friends to read at a memorial held at Natalie’s. The script had stage directions and specific instructions from Brett about who should read each section and even how long to pause so that certain jokes would land. It’s long-winded and rambling — angry at times (“I was ultimately killed by Empty Nose Syndrome and a salesman in a long, white jacket”) and darkly funny at others (“I felt like I was splashing around in the ocean and when Hasselhoff finally pulled up to rescue me, he just slapped some sunscreen on me and drove away on his little Jet-ski”). Brett had a way with words, but it was emotionally torturous for Sean and others to read those words on a stage in front of everyone.
“The idea of selfishly trying to end my suffering seems less and less selfish the worse things get,” Brett wrote. “I beg for your blessing in letting me go… I’m worn out, worn down and nothing feels right anymore. Our bodies are simply not equipped to deal with what I have been dealing with for so long, and I’m really sorry but I gotta get the fuck outta here, you guys.”
The poster from Helling Yeah!, a benefit that Brett’s friends threw to remember him. Courtesy Helling Family
The memorial was so packed that Sean and others had to keep moving tables out of the way to make space for the crowd. He was thankful for the task. It gave him something to do other than sit and stare at that deer head and wonder whether his friend could have been saved.
Brett may get one of his dying wishes in 2016. Though ENS is still little-known to the general public, more ENT doctors are recognizing it and wrestling with it. In August, one of Nayak’s patients, Peter Esquinasi, wrote a letter to the American Rhinologic Society, relaying his ENS experiences and demanding a response. “Just because many people survive these types of surgeries does not mean it is the best thing for them,” he wrote. “Yours is an organization which sadly must answer this question: Do ENTs do extra surgeries for extra money? Or are they grossly misinformed? Either one is bad, but you must look in the mirror and choose one.”
The ARS executive committee responded in a letter. “We want you to know that the American Rhinologic Society is pursuing an ongoing educational effort relating to ENS,” it stated. “Your letter is of particular importance to us in the context of our educational mission.”
Dr. David Poetker, who’s on the ARS board of directors, said in an email that the ARS has no particular stance on ENS. “It is a complex issue that is not very well understood,” Poetker says. “Unfortunately, there is not a lot of money for research for nasal issues in general. We continue to do the best research we can with the limited resources available.”
In January, Dr. Das in Columbus noted a sea change in an open letter to ENS patients he posted on the emptynosesyndrome.org forum. ENS, he said, is the thing keeping some of his colleagues up at night. “There continues to be greater recognition that ENS is a problem,” Das writes. “Many panels within the American Rhinologic Society are discussing ENS as a real problem and leading discussions on the best way to solve this problem.” Das’s letter also expresses hope about the injection therapies he’s tried on 180 patients from 25 countries; 82% of them reported an improvement in their symptoms.
And it’s no small thing that a press release for Ohio State’s nasal surgery study mentions empty nose syndrome by name, even though Carol Helling says Ohio State doctors told Brett he didn’t have it.
In some ways, Brett’s case was typical. His symptoms overlapped with many others who say they have ENS. The problem is, there’s still no firm definition of empty nose syndrome, which means there’s also no firm way of diagnosing it. And misdiagnosis is an issue. Houser and Nayak say they’ve seen patients who were convinced they had ENS but had a different nasal problem entirely.
“My research group is trying to lay the groundwork for better defining ENS, and pulling it out of the ‘mysterious, not sure it exists’ bucket, into the ‘definite diagnosis with defined parameters’ category,” Nayak says. Recently, Nayak and his Stanford researchers analyzed CT scans of patients diagnosed with ENS and compared them to patients who underwent turbinate reduction surgery but had no ENS symptoms — a comparison that had never been done before. “We detected a statistically significant central location in the nasal airway that swells in the CT scans of ENS patients, but not in any control patients,” Nayak says of the soon-to-be-published study. Nayak’s group also came up with six questions he says will more accurately diagnose ENS. He and his team will present their findings at a national meeting of otolaryngologists in Chicago in May.
Doctors’ responses to the presentations could determine how ENT doctors approach ENS moving forward. Will Nayak’s research — along with the work from Ohio State, Das, Houser, and others — finally put the skepticism to rest, or will doubt persist? If the data resonate, will doctors alter their surgical methods? And will those changes spill over to the cosmetic surgery community, where doctors performing nose jobs are probably even less familiar with ENS?
Turbinate reductions aren’t likely to go away, despite outcries of malpractice from ENS patients. Every otolaryngologist I spoke to, including those who acknowledge the dangers of ENS, continues to perform surgeries on turbinates. A friend of Brett’s recently wrote to his congressman to propose a bill that would require doctors to warn patients about the risks of ENS before turbinate surgeries, but even Houser says that goes too far. “The rate of ENS development is so small, and if turbinates are treated properly, ENS should essentially never occur,” Houser says. “The focus should be on educating doctors of proper techniques.”
Houser also often requires patients to undergo mental health assessments before he considers surgery, and Payne says he’s similarly vigilant. “There are some people I’ve refused to do surgery because they were people who I felt were setups for an empty nose scenario,” Payne says.
In January, Brett Helling’s friends celebrated his life with a two-day concert dubbed “Helling Yeah!” at Natalie’s. (The promotional poster featured a giant deer head.) At first, the organizers wanted proceeds from the event to benefit ENS awareness, as well as suicide prevention. But there’s no vetted, surefire way to contribute to ENS awareness yet. Despite the strides in research, it’s still nebulous, still opaque.
Just a couple of weeks before the benefit concert, a frightened new visitor to the Empty Nose Syndrome Facebook page posted a desperate plea.
“Please help! I had surgery December 7, 2015,” she wrote. “I feel the nasal passages as huge tunnels, the cold air burns the nose and throat. … I’m going crazy, no sleep 8 days. What do I do? I don’t want to die.” •



 eved her operative report, it mentioned “full and dwindling septorhinoplasty of inferior turbinates, bilateral”.
eved her operative report, it mentioned “full and dwindling septorhinoplasty of inferior turbinates, bilateral”.














Recent Comments